On this page you will learn about:
Normal or Non-diabetic blood sugar…
Natural insulin (i.e. insulin released from your pancreas) keeps your blood sugar in a very narrow range. Overnight and between meals, the normal, non-diabetic blood sugar ranges between 60-100mg/dl and 140 mg/dl or less after meals and snacks. See the picture below of blood sugar levels throughout the day in someone who does not have diabetes.
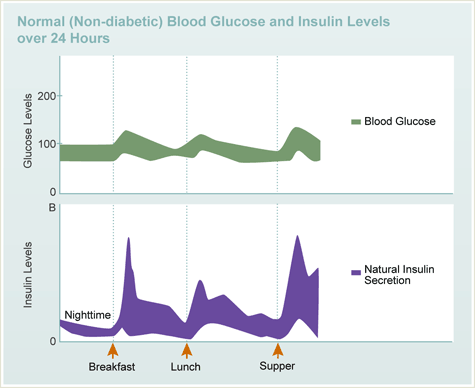 To keep the blood glucose in a narrow range throughout the day, there is a low steady secretion of insulin overnight, fasting and between meals with spikes of insulin at mealtimes. Adapted: Jacobs DM Care 20:1279, 1997
To keep the blood glucose in a narrow range throughout the day, there is a low steady secretion of insulin overnight, fasting and between meals with spikes of insulin at mealtimes. Adapted: Jacobs DM Care 20:1279, 1997
Normal or Non-diabetic insulin release…
To keep the blood sugar controlled overnight, fasting and between meals, your body releases a low, background level of insulin. When you eat, there is a large burst of insulin. This surge of insulin is needed to dispose of all the carbohydrate or sugar that is getting absorbed from your meal. All of this happens automatically! Insulin is continuously released from the pancreas into the blood stream. Although the insulin is quickly destroyed (5-6 minutes) the effect on cells may last 1-1/2 hours. When your body needs more insulin, the blood levels quickly rise, and, the converse – when you need less, the blood levels rapidly fall.
When you have type 1 diabetes…
The situation is different when you have diabetes and are getting insulin replacement therapy. Once you have injected a dose of insulin, it is going to get absorbed into your bloodstream whether you need it or not.
Normal or Non-diabetic insulin release…
At mealtime, a little insulin is released even as you are first smelling or chewing the food. This gets your body ready to receive the sugar load from the meal. Then as you eat and the food is digested, the sugar levels rise which causes a surge of insulin. The insulin levels rapidly climb and peak in about 45 minutes to 1 hour before falling back to the background or basal levels.
When you have type 1 diabetes…
The situation is different when you have diabetes and are getting insulin replacement therapy. You have to calculate how much carbohydrate you are going to eat and how much insulin you will need. And you have to try to mimic natural overnight, fasting (or between meals) and mealtime insulin release with injected insulin.
Principles of insulin replacement
When you have type 1 diabetes, you will need to start insulin therapy because you no longer make your own insulin. The insulin therapy tries to mimic natural or non-diabetic insulin secretion. There are two components of insulin therapy.
1. Background or basal insulin replacement
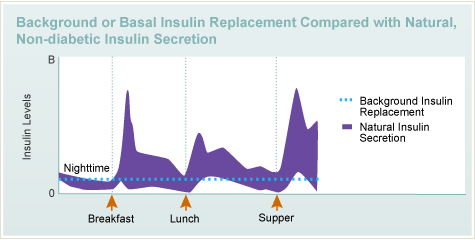 Intensive insulin therapy tries to duplicate the body’s natural pattern of insulin secretion. With intensive insulin therapy you need a low steady amount of insulin overnight, while fasting and between meals as illustrated by the dashed line. Adapted: Jacobs DM Care 20:1279, 1997
Intensive insulin therapy tries to duplicate the body’s natural pattern of insulin secretion. With intensive insulin therapy you need a low steady amount of insulin overnight, while fasting and between meals as illustrated by the dashed line. Adapted: Jacobs DM Care 20:1279, 1997
Basal Replacement:
- Controls glucose overnight and between meals by keeping fat in fat tissue and curbing glucose production from the liver.
- Provides a low, continuous level of insulin.
- Can be a long-acting insulin, which you inject once or twice daily such as the insulin analogs, insulin glargine, insulin detemir and NPH.
- Or can be a rapid-acting insulin continuously infused under the skin, if you are using an insulin pump.
- Represents about 50% or half of the body’s daily insulin requirements.
2. Bolus insulin replacement
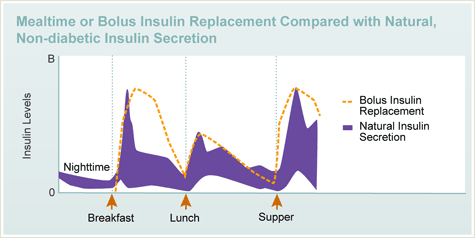 Intensive insulin therapy tries to duplicate the body’s natural pattern of insulin secretion. With intensive insulin therapy you need a rapid surge of insulin at mealtimes as illustrated by the golden lines. Adapted: Jacobs DM Care 20:1279, 1997
Intensive insulin therapy tries to duplicate the body’s natural pattern of insulin secretion. With intensive insulin therapy you need a rapid surge of insulin at mealtimes as illustrated by the golden lines. Adapted: Jacobs DM Care 20:1279, 1997
There are two kinds of bolus replacement:
- Mealtime Bolus – to cover the carbohydrate in the meal or snack.
- High Blood Sugar Correction Bolus – provides extra insulin to return the blood sugar back to the target level when your blood sugar is too high.
- Bolus Insulin is usually provided by a rapid-acting insulin analogs, such as insulin aspart, insulin Lyspro, and insulin glulisine or Regular insulin.
- Represents about 10% to 20% of the daily insulin requirement at each meal, or about 50% of the body’s daily insulin needs.
Read about the different types and characteristics of insulinthat are suitable for basal and bolus insulin.
Learn more about :
- Types and characteristic of insulin medications
- Insulin administration
- Designing an insulin regimen
- Calculating your insulin dose
- Intensive insulin therapy
- Insulin pump therapy
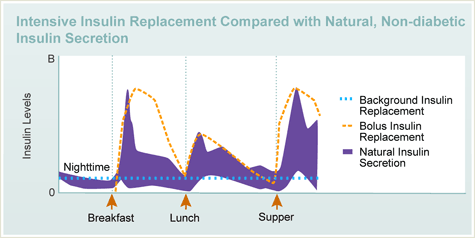 Intensive insulin therapy tries to duplicate the body’s natural pattern of insulin secretion. With intensive insulin therapy you need a low steady level of insulin overnight, fasting, and between meals, and a rapid surge of insulin at mealtime. Adapted: Jacobs DM Care 20:1279, 1997
Intensive insulin therapy tries to duplicate the body’s natural pattern of insulin secretion. With intensive insulin therapy you need a low steady level of insulin overnight, fasting, and between meals, and a rapid surge of insulin at mealtime. Adapted: Jacobs DM Care 20:1279, 1997
Self-assessment Quiz
Self assessment quizzes are available for topics covered in this website. To find out how much you have learned about Treatment of Type 1 Diabetes, take our self assessment quiz when you have completed this section. The quiz is multiple choice. Please choose the single best answer to each question. At the end of the quiz, your score will display. If your score is over 70% correct, you are doing very well. If your score is less than 70%, you can return to this section and review the information.
