What is an intensive insulin regimen?
Intensive insulin regimens attempt to mimic the body’s normal pattern of insulin secretion, and deliver replacement insulin using the concepts of basal and bolus insulin coverage.
When you are intensively managed with insulin your medical provider will prescribe an insulin regimen for you, but these are the general principles:
Your insulin regimen will include:
- A basal or background insulin dose
- A bolus insulin dose to cover the sugar or carbohydrate in your food
This will be presented as an insulin to carbohydrate ratio (I:CHO). The I:CHO tells you how many grams of carbohydrate can be covered by one unit of rapid acting insulin - A high blood sugar correction bolus insulin dose to bring your blood sugar back into the target range. This will be presented as a correction factor. This correction factor refers to how much your blood sugar will drop after 1 unit of insulin rapid acting insulin.
Intensive insulin therapy requires:
- Multiple daily injections of insulin (MDI), or
- Insulin pump therapy
With MDI, glargine, detemir or NPH is used to provide basal (background) insulin; and insulin aspart, glulisine, lispro or Regular provide bolus (mealtime and high blood sugar correction) coverage.
With an insulin pump, insulin aspart, glulisine or lispro provide both basal and bolus insulin replacement.
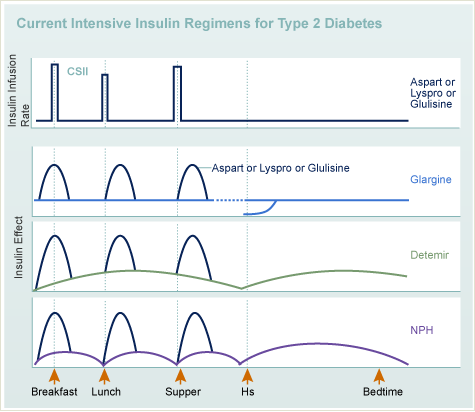
INTENSIVE INSULIN THERAPY: INJECTIONS OR PUMPS TO MIMIC THE BODY’S NATURAL SYSTEM
Advantages of Intensive Insulin Regimens
- While intensive regimens require more calculation at each meal, they allow for more flexibility in timing and in the amount of carbohydrate content in meals and snacks.
- An accurate insulin dose will also result in better blood glucose control with fewer high and low blood sugars.
- Changes in activity and stress can be accommodated without sacrificing glucose control.
- Over time, high blood glucose correction can be separated from the food coverage. For example, if your blood sugar is very high (over 240 mg/dl), you can delay your meal and give yourself a correcting dose. Once your blood sugar falls below 200 mg/dl, you can inject your meal insulin and then eat.
- Learning these important skills will make managing your diabetes easier.
Skills check list for intensive insulin therapy:
- Monitor your blood-glucose
(minimum: pre-meal, bedtime, when experiencing a low blood glucose and before driving) - Count your carbohydrates
- Know your insulin formula
(insulin-to-carbohydrate ratio, blood glucose correction, background dose) - Understand how different insulin formulations act in your body
- Establish blood sugar goals
(pre meal, post meal, bedtime) - Know how to troubleshoot when your blood sugar is not at your goal
- Understand glucose emergency responses
(such as what to do for low and high blood sugars, and when to check ketones and use glucagon)
Self-assessment Quiz
Self assessment quizzes are available for topics covered in this website. To find out how much you have learned about Insulin Therapy, take our self assessment quiz when you have completed this section. The quiz is multiple choice. Please choose the single best answer to each question. At the end of the quiz, your score will display. If your score is over 70% correct, you are doing very well. If your score is less than 70%, you can return to this section and review the information.
