- How do you treat type 2 diabetes?
- Can type 2 diabetes go away? If my blood sugar becomes normal, do I still have diabetes?
- Will I need to take insulin if I have type 2 diabetes?
- As someone with type 2 diabetes, do I turn into a type 1 diabetic when I take insulin?
- If I have type 2 diabetes and take insulin, do I have to take it forever?
- Will exercise help my diabetes?
- If I have type 2 diabetes, can I stop taking diabetes medications if I eliminate candy and cookies from my diet?
- Do I need to monitor my blood sugar when I have type 2 diabetes?
- Are my children at risk?
- Can type 2 diabetes be prevented?
How do you treat type 2 diabetes?
When you have type 2 diabetes, you first need to eat a healthy diet, stay physically active and lose any extra weight. If these lifestyle changes cannot control your blood sugar, you also may need to take pills and other injected medication, including insulin.
Eating a healthy diet, being physically active, and losing any extra weight is the first line of therapy. “Diet and exercise“ is the foundation of all diabetes management because it makes your body’s cells respond better to insulin (in other words, it decreases insulin resistance) and lowers blood sugar levels.
If you cannot normalize or control the blood sugars with diet, weight loss and exercise, the next treatment phase is taking medicine either orally or by injection.
Diabetes pills work in different ways – some lower insulin resistance, others slow the digestion of food or increase insulin levels in the blood stream. The non-insulin injected medications for type 2 diabetes have a complicated action but basically lower blood glucose after eating. Insulin therapy simply increases insulin in the circulation.
Don’t be surprised if you have to use multiple medications to control the blood sugar. Multiple medications, also known as combination therapy is common in the treatment of diabetes! If one medication is not enough, you medical provider may give you two or three or more different types of pills. Insulin or other injected medications also may be prescribed. Or, depending on your medical condition, you may be treated only with insulin or injected medication therapy.
Many people with type 2 diabetes have elevated blood fats (high triglycerides and cholesterol) and blood pressure, so you may be given medications for these problems as well.


Can type 2 diabetes go away? And if my blood sugar becomes normal, do I still have diabetes?
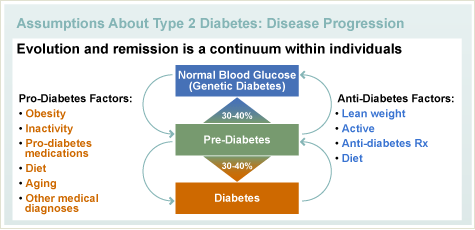
Type 2 diabetes is a genetic condition or pre-disposition that doesn’t change with treatment. But diabetes is defined as an elevated blood sugar.
When your blood sugar is normal with no treatment, then the diabetes is considered to have gone away. However, even when the blood sugars are controlled, because type 2 diabetes is a genetic condition, the predisposition for diabetes always exists. High blood sugars can come back.
If you have type 2 diabetes and the blood sugar is controlled during treatment (diet, exercise and medications), it means that the treatment plan is working. You are getting the good blood sugar because of the treatment – NOT because diabetes predisposition has gone away. You will need to continue your treatment; otherwise your blood sugar will go back up.
Will I need to take insulin if I have type 2 diabetes?
Maybe. Historically, 30% or more of people with type 2 diabetes required insulin therapy. However there are many new drugs available that may delay or prevent the need for insulin therapy. It is expected that fewer and fewer individuals will need insulin replacement to control their blood sugars.
As someone with type 2 diabetes, do I turn into a type 1 diabetic when I take insulin?
No. Taking insulin does not mean that you have type 1 diabetes. Your type of diabetes is determined by your genetics, not by the type of therapy.
If I have type 2 diabetes and take insulin, do I have to take it forever?
Not necessarily. If you can lose weight, change your diet, increase your activity level, or change your medications you may be able to reduce or stop insulin therapy. Under certain circumstances, you may only need insulin temporarily – such as during pregnancy, acute illness, after surgery or when treated with drugs that increase their body’s resistance to the action of insulin (such as prednisone or steroids). Often the insulin therapy can be stopped after the event or stress is over.
Will exercise help my diabetes?
Exercise is very beneficial in the management of type 2 diabetes. Always consult with your doctor about exercise guidelines, to exercise safely and reduce risks.
If I have type 2 diabetes can I stop taking diabetes medications if I eliminate candy and cookies from my diet?
If you eliminate concentrated sources of carbohydrates (foods that turn into sugar in your blood stream) like candy and cookies, you may be able to reduce or eliminate the need for diabetes medications. Everyone with type 2 diabetes will benefit from an improved diet, but you may still need other interventions, such as increased physical activity, weight loss or medications to keep your blood sugars in the target range. Check with your doctor about any diabetes medication dose adjustments that may be required if you change your diet.
Do I need to monitor my blood sugar when I have type 2 diabetes?
You may feel fine, but that is no guarantee that your blood sugar levels are in the target range. Remember, diabetic complications do not appear right away. And complications may develop even when the blood sugar is only slightly elevated. Regular blood sugar monitoring can help you keep your blood sugars in control and prevent serious damage to your eyes, kidneys and nerves. If your sugar levels are out of line, consult your doctor.
Yes. Type 2 diabetes is a genetic disease. The risk is highest when multiple family members have diabetes, and if the children also are overweight, sedentary and have the other risk factors for type 2 diabetes. Your child has a 10-15% chance of developing type 2 diabetes when you have type 2 diabetes. And if one identical twin has type 2 diabetes, there is a 75% likelihood of the other twin developing type 2 diabetes also.
Can type 2 diabetes be prevented?
Results of the Diabetes Prevention Program-DPP
Although we cannot change your genetic risk for developing type 2 diabetes, we do know that even modest exercise and weight loss can delay or prevent the development of type 2 diabetes. A landmark research study in the United States, the Diabetes Prevention Program (DPP) was completed in 2002 and showed that when people modified their risk factors for type 2 diabetes, they reduced their chance of developing the condition. Similar results have been shown in Finland.
In the DPP study, people with pre-diabetes were enrolled and assigned to 3 different treatments:
- Intensive lifestyle changes – exercise (30 minutes, 5 days a week), a healthy diet, and weight loss (loss of 7% of initial weight)
- The diabetes drug, Metformin
- An inactive placebo disguised as Metformin
The group that made lifestyle changes was 58% less likely to develop diabetes compared to the placebo group. And the group that took Metformin was 31% less likely to develop diabetes compared to the placebo group. In other words – lifestyle changes and Metformin therapy can delay or prevent the onset of type 2 diabetes. Lifestyle changes (weight loss, healthy diet and activity) are the most effective intervention.
Self-assessment Quiz
Self assessment quizzes are available for topics covered in this website. To find out how much you have learned about Facts about Diabetes, take our self assessment quiz when you have completed this section. The quiz is multiple choice. Please choose the single best answer to each question. At the end of the quiz, your score will display. If your score is over 70% correct, you are doing very well. If your score is less than 70%, you can return to this section and review the information.
