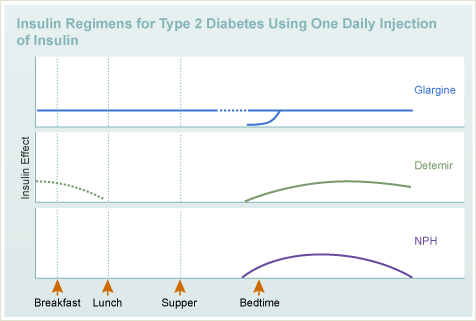
The main goal in designing an insulin regimen is to mimic how the body normally releases insulin. If you have type 2 diabetes, there are two main ways to replace insulin. Intensive Insulin Therapy closely mimics the natural insulin production. The second, referred to as Conventional or Sliding Scale Insulin Therapy, more loosely approximates insulin needs.
For Intensive Regimens:
When you are intensively managed with insulin your medical provider will prescribe an insulin regimen for you, but these are the general principles:
Your medical provider should prescribe:
- A basal or background insulin dose
This will be prescribed as one or two injections of long acting insulin, or, if you are using an insulin pump, a daily infusion rate of continuous, small amounts of rapid acting insulin. The background/basal insulin dose is usually the same day to day. With an insulin pump you do have the option of temporarily changing the background rate for a few hours – up or down as needed! - A bolus insulin dose to cover the sugar or carbohydrate in your food
This will be presented as an insulin to carbohydrate ratio( I:CHO). The I:CHO ratio tells you how many grams of carbohydrate can be covered by one unit of rapid acting insulin. You will need to calculate how much carbohydrate you will eat, and take a dose of insulin that matches the food. - A bolus insulin dose to bring your blood sugar back to the normal range
A high blood sugar correction bolus insulin dose to bring your blood sugar back into the target range. This will be presented as a correction factor. This correction factor refers to how much your blood sugar will drop after 1 unit of insulin rapid acting insulin. When your blood sugar is too high, you will need to calculate how much your blood sugar is over the target, and, based on the correction factor, then the dose of insulin that will bring you down into the desired range.
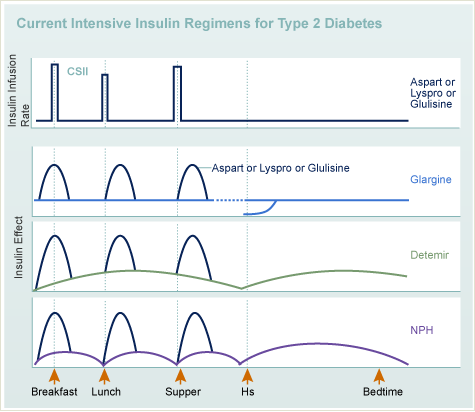
Common intensive regimens for type 2 diabetes:
- Long-acting insulin (glargine/detemir) once or twice a day with rapid acting insulin (Aspart, glulisine, lispro) before meals and as need to correct high blood sugars.
- Rapid acting insulin (Aspart, glulisine, lispro) delivered via an insulin pump.
- Three small doses of NPH before meals, and a larger dose of NPH at night , with rapid acting insulin (aspart, glulisine, lispro) before meals and, as needed, for snacks and to correct high blood sugars.
For more information, please refer to the following sections:
For Sliding Scale Therapy
You should be prescribed:
- A “sliding scale” insulin dose
The insulin dose is based on your blood sugar. The higher the blood sugar, the higher the insulin dose. – and visa versa. The lower your blood sugar, the loser the insulin dose. Sliding scale insulin regimens approximate daily insulin requirements.
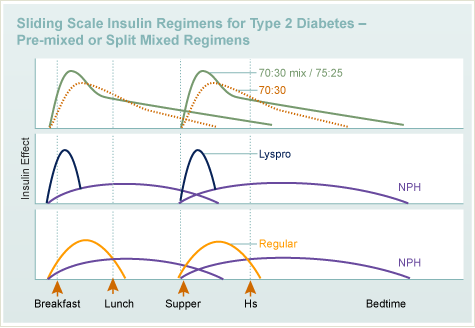
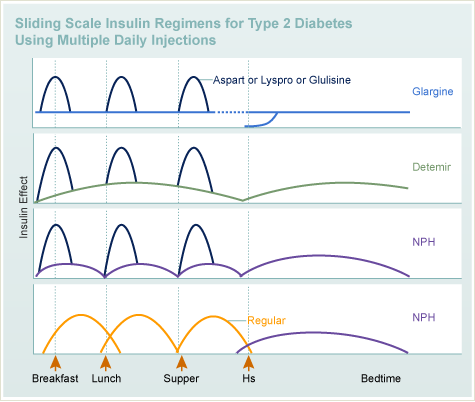
Common sliding scale regimens:
- Long-acting insulin (glargine/detemir or NPH) once or twice a day with short acting insulin (aspart, glulisine, lispro, Regular) before meals and at bedtime.
- Long-acting insulin (glargine/detemir or NPH) given once a day
- Regular and NPH given twice a day
- Pre-mixed, short-acting insulin analogs or Regular and NPH given twice a day
For more information, please refer to the following sections:
Self-assessment Quiz
Self assessment quizzes are available for topics covered in this website. To find out how much you have learned about Insulin Therapy, take our self assessment quiz when you have completed this section. The quiz is multiple choice. Please choose the single best answer to each question. At the end of the quiz, your score will display. If your score is over 70% correct, you are doing very well. If your score is less than 70%, you can return to this section and review the information.